READING SUMMARY: The American Society of Addiction Medicine recommends AGAINST the practice of rapid detox due because it is an unproven treatment method with many health risks. Even if rapid detox works for some people, there are safer, and more effective alternatives to overcome drug dependence.
TABLE OF CONTENTS
What Is Rapid Detox?
The idea of a less uncomfortable, “rapid detox” was developed about 20 years ago by detox specialists who hoped to ease the discomfort of withdrawal and decrease the overall time spent in detox. Basically, treatments for opiate withdrawal called “detox under anesthesia” or “rapid opiate detox” involve placing you under anesthesia and injecting large doses of opiate-blocking drugs to your system. The idea is that the opiate blockers will speed up the return to normal opioid system function.
During the procedure, doctors first administer a general anesthetic for sedation. Then, they administer a medicines like naltrexone to trigger symptoms of withdrawal. After 4-6 hours you wake up … but detox has just started.
In general, withdrawal from opiates is unpleasant, uncomfortable, and temporarily painful. So, is this alternative way to withdraw from drugs effective or safe? More on the efficacy of ultra-rapid opiate detoxification (a.k.a. UROD) follows. We’ll review its safety so that you can evaluate the option before you “go under” this procedure.
Does It Work?
The main intention of rapid detox is to help people get opiate drugs out of their system. Rapid detox is widely advertised for detox from stronger opiates like:
- codeine
- hydrocodone
- heroin
- morphine
- oxycodone
As people withdraw and remove the drugs from their system, they prefer to be drowsy and sedate. In fact, the main reason why users are eager to try this method is because they want to avoid the withdrawal discomfort. Some people even view rapid detox as a magical way to skip the entire detox protocol and energy they have to invest in order to get the quick results.
However, the truth is that addiction is a disease that requires a step-by-step approach working on the mental and physical aspects of the condition.
The National Institute on Drug Abuse NIDA reported and published this study in 2006 comparing 3 different types of detox. The summary compared detox efficiency for over 100 patients and found anesthesia-assisted detox to be no more easier than other approaches. Further, the American Society of Addiction Medicine DOES NOT recommend rapid detox due to the fact that it is an unproven treatment method with many health risks.
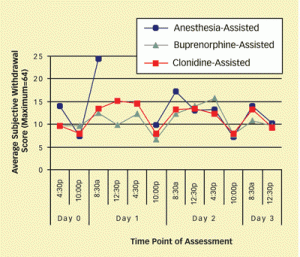
Duration
The whole procedure of rapid detox only takes a few days, but the road to recovery be difficult. In fact, patients in this study who went through ultra-rapid detox showed the highest rate of withdrawal symptoms at one hour after anesthesia. While most of detox symptoms subsided after 24 hours, the underlying issues that drive drug use are still present.
A person undergoing rapid detox will also need residential treatment, or outpatient services. Since relapse is common in opiates addiction, the chances are very big that people who go through this “immediate solution” might go back to using again. Therefore, rapid opiate detox may take only 72 hours, but should be followed by 3-6 months of rehabilitation programs and up to 1 year or more of follow up therapy for best results.
Cost
Rapid detox is expensive.
Depending on the course of treatment, this procedure may cost you between$10,000-15,000. The process is done in the hospital and because sedation and intensive monitoring are involved, the costs can be even higher. Another financial inconvenience is the fact that insurance companies do not cover the costs of rapid detox because it is not considered to be medically safe.
Effectiveness
Doctors continue to use techniques developed during rapid detox because, in a sense, the technique does work to move withdrawal and detox along. Plus, treatment outcomes are similar to other types of detox protocols (buprenorphine or clonidine assisted detox). But some of the claims that detox centers make are pure advertising, and have not been proven in clinical trials.
In fact, the risks and the costs of rapid opiate detox are real. And as much as you might like the idea of sleeping through withdrawal, you need to know the facts about this procedure. We present them here.
- Rapid opiate detox does not decrease time in detox.
There is no evidence that ultra-rapid opiate detoxification programs actually reduce the time you spend in withdrawal.
- Rapid opiate detox does not decrease intensity of withdrawal symptoms.
In some cases, rapid detox may reduce the intensity of symptoms during general anesthesia and the immediate recovery period. But in most cases, once awakened from anesthesia, people who choose ultra rapid detox report symptoms of discomfort comparable to those of more conventional detox procedures using buprenorphine or clonidine assisted detox.
- Rapid opiate detox is medically risky.
There have been several deaths associated with detox under anesthesia, particularly when performed outside a hospital. Rapid detox can provoke unconsciousness, transient confusion, or depressive mood. Or even worse. Pulmonary, psychiatric complications, and metabolic complications from diabetes, all of which require hospitalization are possible. Of particular concern is vomiting during anesthesia (opiate withdrawal produces vomiting).
Because of the significant increase in death risk, many specialists think the risks of rapid opiate detox outweigh the potential and unproven benefits.
Dangers
Adverse events including life threatening situations are a serious consequence of opiate detox. These risky outcomes may result in significant negative impact over people’s health and well-being while the drugs are being removed from the system. The many risks associated with this approach include
- fluid accumulation in the lungs
- metabolic complications of diabetes
- worsening of underlying bipolar illness
…as well as other potentially serious adverse events. People with preexisting medical conditions are particularly at risk for anesthesia-related adverse events. Preexisting medical conditions that put you more at risk of adverse events include:
- elevated blood sugar levels
- insulin-dependent diabetes
- psychiatric disorders
- prior experience of pneumonia, hepatitis, heart disease, or AIDS
In fact, addiction experts have raised several concerns about the serious adverse events, including death, related to rapid and ultra-rapid opiate detoxification. According to this 2013 report from the Centers for Disease Control, a number of incidents have been noted among which several deaths and numerous more near-deaths during rapid detox.
NOTE HERE: While rapid detox is presented as an alternative to traditional detox, know that it is NOT safe.
Still Have Questions?
Experts agree that there is no compelling reason for using general anesthesia to treat opiate dependence, especially as it presents particular safety concerns. Instead, when you are ready to detox from opiates, talk to your doctor first about how to slowly stop prescription medicine or how to taper doses gradually to prevent signs and symptoms of withdrawal. Then, you can check in to a medically supervised detox center to get opiates out of your system.
If you have any additional questions about opiate rapid detox, or would just like to share your experience, don’t hesitate to leave a comment below. We love to hear from our readers, and we look forward to helping you move forward to a drug-free life.










Related Posts